Breastfeeding Success In The Early Days: A rewarding and challenging experience awaits!
You have decided to breastfeed, congratulations, this article will set you on the road to Breastfeeding Success.
Exclusive breastfeeding is recommended for a baby for the first six months or longer unless your baby has a medical reason otherwise. This means your baby gets only breastmilk, not other fluids, like formula, water, or foods.
See also: 15 Safe Sleep Tips for Baby
Colostrum—baby’s First Food
During the first few days after birth, your breasts make colostrum—food so rich in nutrients and infection-fighting antibodies that it’s called liquid gold. It’s all your newborn needs.
Breastfeeding—A Learned Experience
From the first latch, you and baby learn about breastfeeding. For many moms and babies, especially first-timers, this process takes patience, rest, family support and a healthy diet with plenty of water. Breastfeeding success can take time and patience.
Help your Breastfeeding Success: Nurse-Recommended breastfeeding positions and also Top 5 Breastfeeding Positions
The Golden Hour—The First-Hour Post-Birth
Baby should be placed on your chest, skin-to-skin, at birth, to promote bonding and breastfeeding success. Babies are most alert and awake in the first hour. Your nurse will help you bring baby to latch onto the areola—the darkened area around the nipple—with a wide-open mouth.
ALSO READ: Breastfeeding & Pumping at Work
The First 24 Hours of Life
Babies are often sleepy after the first feeding and for the next 24 hours. Keep baby close-by, skin-to-skin if possible, to help you learn how baby shows interest in nursing. Crying is a late cue; a crying baby may need calming before latching. Expect your baby to breastfeed at least 8-10 times in a 24-hour period. Let baby nurse “on-demand”. The more baby nurses, the sooner your milk comes in.
See also: Pregnant During COVID-19
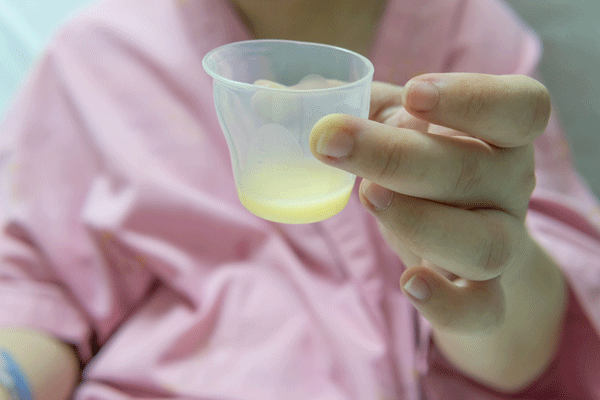

When Will My Milk Come in?
Colostrum changes to milk by days 2 to 5. You may have engorgement—full-feeling breasts—when your milk comes in which should resolve in 24-48 hours. For tender breasts apply warm compresses before nursing, gently massaging as you nurse. If baby has difficulty latching, express some milk before feeding by placing your thumb above the areola, your fingers below, and gently pressing to release some milk.
How Do I Know my Baby is Getting Enough?
Baby’s diaper tells all! Look for one wet diaper and one stool on day 1, with two of each on day 2, and three each on day 3. Stools are black and tarry at first and then turn yellow and seedy. By day 4, expect baby to wet the diaper and pass stool each time you nurse. If your baby isn’t producing this much urine and stool talk to baby’s provider right away.
Listen to your Intuition!
Mom—you’ve got this!
For expert advice ask your nurse, healthcare provider, and/or a lactation counselor/consultant. La Leche League USA (lllusa.org) can be a helpful resource.
We also have many articles that will help you on your way to Breastfeeding Success, just click here to go to our Breastfeeding section.






Comments are closed.